Telehealth Interoperability in Clinical Systems
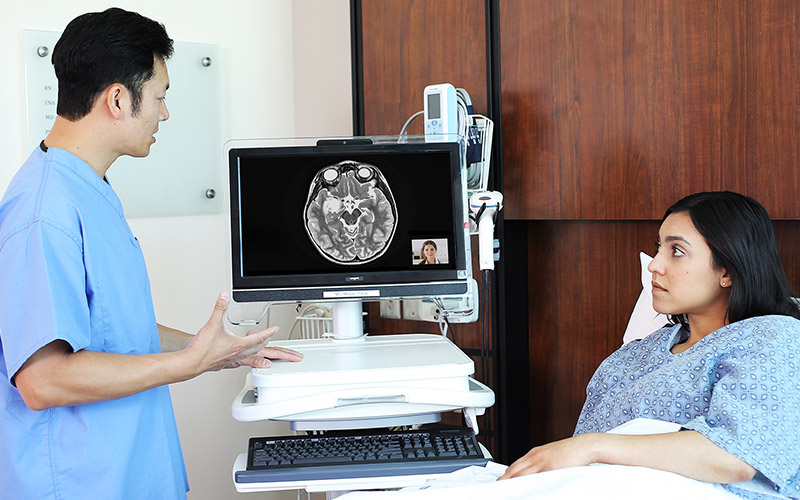
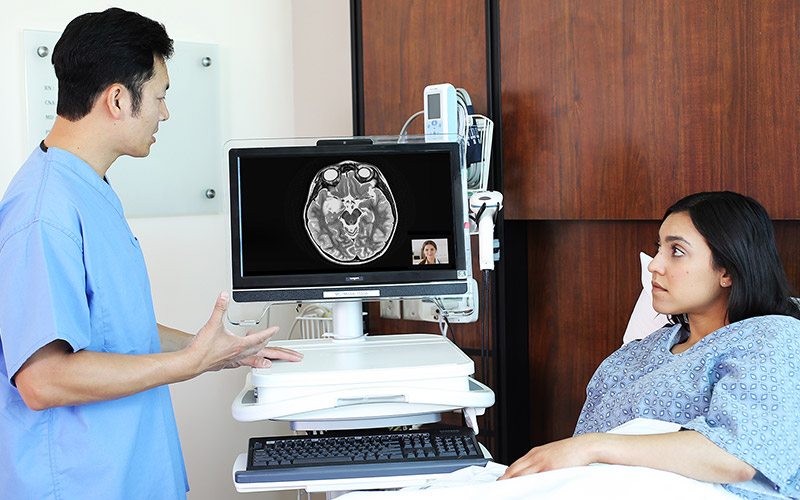
Adding real-time video capabilities to your organization’s telehealth workflow can provide a wealth of benefits for both your patients and providers. In fact, we dedicated an entire section in our latest report, Making Telehealth Work for You: The Ultimate Guide, to infrastructure and interoperability. But executing an organic, satisfying experience for both parties can prove challenging, hindering adoption of the service and diminishing the value of some — if not all — of the possible benefits.
In this first in a series of blog posts regarding telehealth interoperability with clinical systems (such as Epic, Cerner, and Allscripts) and operational support systems (such as Telehealth Management TRP), we’ll cover why it’s imperative that the telehealth solution you choose have a robust interoperability layer. We’ll also discuss some of the issues that can be caused by the lack of telehealth interoperability.
Increased clinician buy-in
Clinicians want to get right to the patient examination. They want ease of use. What they don’t want is to wrestle with technology or have to open many screens on their device to see the necessary patient information. Give your providers a seamless workflow and you’ll experience increased clinician adoption of virtual care and deeper integration of it in their practice.
Increased patient population buy-in
Greater telehealth interoperability in clinical systems gives your patients a convenient, easy-to-use workflow. Today’s patients are accustomed to the idea of digital transactions and expect simplicity and elegance as consumers. To maximize patient adoption, keep the user experience top of mind. Today’s consumers will not accept a frustrating learning curve that requires multiple apps to complete a transaction.
Improved care coordination and continuity of care
Your organization will be able to provide more comprehensive analytics because telehealth-delivered care data can be aggregated with all patient data. The availability of comprehensive patient data at the point of care will likely lead to better, faster, and more comprehensive care and better outcomes. This can be especially true with mobile platforms. Finally, your provider team will be able to offer enhanced population health management — a critical driver for value-based reimbursement.
So what are some of the possible issues you may encounter if your clinical systems are not interoperable with your virtual care systems?
- Lack of pertinent patient data at the point of care
- Low patient engagement and adoption
- Unnecessary extra steps or clicks for clinicians
- Inability to coordinate care
- Siloed telehealth-related data
- Onerous learning curves for clinicians and patients
I’ve seen both the benefits and challenges that can be experienced when implementing telehealth services. Vidyo’s video communication platform fosters an effective, personal connection between providers and patients and has a robust interoperability layer. In the coming posts, we’ll show you specifically what you need to do in order to create seamless and successful interoperability with the major EHRs (think: Epic, Cerner, Allscripts) and other clinical and operational systems.